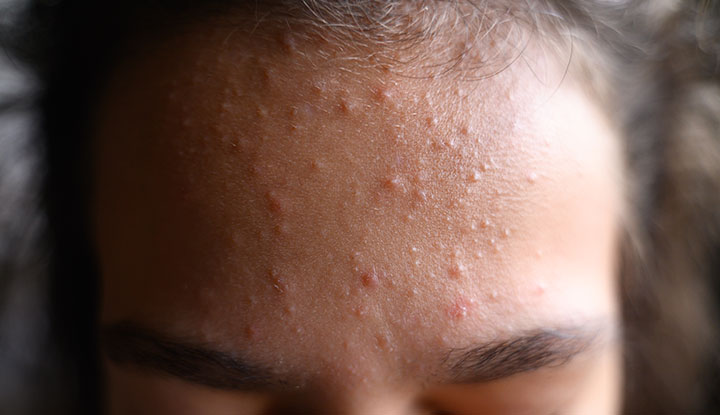
Few things are as maddening as lying in bed, exhausted and ready to sleep, only to have your skin erupt in an itch you can’t locate, can’t explain, and can’t stop. Widespread itching that worsens at night—with or without a visible rash—is a real medical symptom with a long list of potential causes.
When you are dealing with unexplained itching all over body at night (clinically known as nocturnal pruritus), the triggers can range from simple environmental factors to internal systemic issues. This discomfort is most commonly caused by dry skin, eczema, allergic reactions to laundry detergents, liver or kidney conditions, thyroid imbalances, or in some cases, blood disorders. When there’s no visible rash, it’s called “pruritus sine materia”—itch without a visible skin change—and it warrants a proper medical workup if it persists for more than two weeks.
Why Does Itching Get Worse at Night?
There are real physiological reasons why skin itches more after dark:
- Body temperature rises at night – warmth triggers histamine release, which causes itching
- Skin loses more moisture overnight – natural trans-epidermal water loss peaks, causing dryness
- Cortisol (anti-inflammatory hormone) is lower at night – so inflammatory responses are less suppressed
- Distractions disappear – without daytime stimulation, the brain amplifies itch signals
- Circadian rhythm of immune cells – mast cells (which release itch-causing histamine) are more active at night
Common Causes of Nighttime Whole-Body Itching
Dry Skin (Xerosis)
The most common cause – especially in older adults and during winter months when heating systems reduce indoor humidity. Dry skin has no rash, but causes an intense crawling, tight, itchy sensation all over.
Clues: Worse in winter, relieved by moisturizing, skin feels tight or flaky.
Eczema (Atopic Dermatitis)
Eczema commonly flares at night. It causes intense itching – often in patches – with red, inflamed, sometimes scaly skin. The nocturnal itch cycle of eczema (itch → scratch → inflammation → more itch) is one of its most disruptive features.
Psoriasis
Similar to eczema in its nocturnal flaring. Psoriasis patches are typically well-defined, thickened, and silvery-scaled – often on the elbows, knees, scalp, and torso.
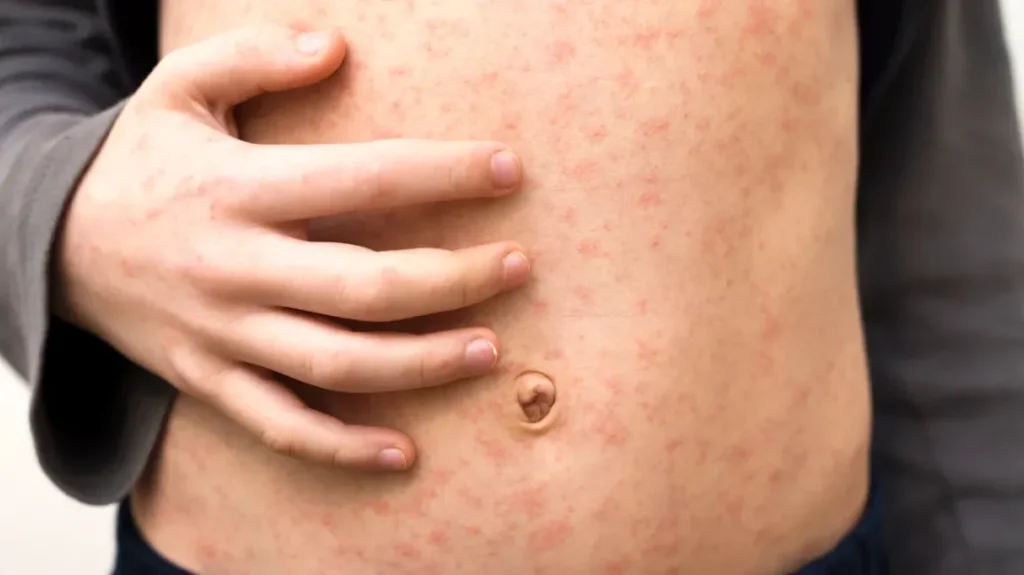
Allergic Reactions / Contact Dermatitis
Reaction to a new detergent, soap, fabric, lotion, or food can cause widespread itching – sometimes with a rash, sometimes without. Common nighttime triggers: fabric softener on bedding, laundry detergent residue, new pajamas or bedsheets.
Liver Disease (Cholestasis)
When bile flow is impaired (from liver disease, gallstones, or intrahepatic cholestasis), bile salts accumulate in the skin – causing intense itching, often worst at night. This type of itch can be severe and is not relieved by antihistamines.
Other signs: Jaundice, dark urine, pale stools, fatigue.
Kidney Disease (Uremic Pruritus)
Kidney failure leads to toxin buildup in the blood, which can cause widespread, severe itching – particularly at night. This is one of the most distressing symptoms of advanced kidney disease.
Thyroid Disorders
Both overactive (hyperthyroid) and underactive (hypothyroid) thyroid function can cause skin changes and itching. Hypothyroidism causes dry, itchy skin; hyperthyroidism can cause widespread itching through increased blood flow and skin sensitivity.
Iron Deficiency Anemia
Low iron affects skin health and can cause itching, sometimes before anemia itself is clinically apparent. The mechanism isn’t fully understood but is well-documented.
Polycythemia Vera
A blood disorder where the body produces too many red blood cells. Itching – particularly after a warm shower or bath (aquagenic pruritus) – is a classic and often early symptom.
Hodgkin’s Lymphoma
Widespread itching, especially at night, is a recognized early symptom of Hodgkin’s lymphoma. Known as a “B symptom,” it warrants investigation when it’s persistent and unresponsive to treatment, particularly alongside night sweats and unexplained weight loss.
Diabetes
Poorly controlled blood sugar can cause widespread itching through skin dryness, peripheral neuropathy, and reduced immune function.
Medications
Many common medications cause itching as a side effect or allergic response: opioids, ACE inhibitors, diuretics, statins, and some antibiotics.
Associated Symptoms and What They Suggest
| Symptom Alongside Itching | Possible Cause |
|---|---|
| Yellow skin or eyes | Liver disease |
| Night sweats + weight loss | Lymphoma or other systemic condition |
| Dark urine, pale stools | Bile duct obstruction |
| Itching after shower/bath (warm water) | Polycythemia vera |
| Itching only in winter, no rash | Dry skin |
| Fatigue + cold sensitivity | Thyroid disorder |
| Excessive thirst + frequent urination | Diabetes |
Immediate Relief for Nighttime Itching
While working out the cause:
- Moisturize heavily at night – use a thick cream or ointment (not lotion) right after bathing; seal moisture into the skin
- Keep the bedroom cool – lower temperature reduces histamine-triggered itch
- Use fragrance-free bedding and laundry products
- Try a cool compress on the worst areas
- OTC antihistamines (diphenhydramine/Benadryl) at night may help, though they don’t address the underlying cause
- Menthol-containing lotions create a cooling sensation that temporarily overrides itch signals
When to See a Doctor
Don’t wait if:
- Itching has lasted more than 2 weeks with no obvious cause
- It’s affecting your sleep significantly
- No rash is visible (unexplained itch without rash is more concerning than itching with a rash)
- You have any of the associated symptoms in the table above
- You’ve lost weight unexpectedly or have night sweats
A doctor will typically order: full blood count, liver function tests, kidney function, thyroid panel, blood glucose, and iron studies. These tests cover the most common internal causes.
Bottom Line
Nighttime itching all over the body is not something to just tolerate indefinitely. While dry skin and eczema account for most cases, persistent unexplained nocturnal itching – especially without a visible rash – can be a window into something systemic. Keep a symptom diary, moisturize aggressively in the meantime, and get blood work done if it’s been going on for more than two weeks.